- Therapeutic Cataract & Refractive
- Lens Technology
- Glasses
- Ptosis
- AMD
- COVID-19
- DME
- Ocular Surface Disease
- Optic Relief
- Geographic Atrophy
- Cornea
- Conjunctivitis
- LASIK
- Myopia
- Presbyopia
- Allergy
- Nutrition
- Pediatrics
- Retina
- Cataract
- Contact Lenses
- Lid and Lash
- Dry Eye
- Glaucoma
- Refractive Surgery
- Comanagement
- Blepharitis
- OCT
- Patient Care
- Diabetic Eye Disease
- Technology
Update on iris melanoma
Case study shows multiple factors determine best course of treatment for this rare disease
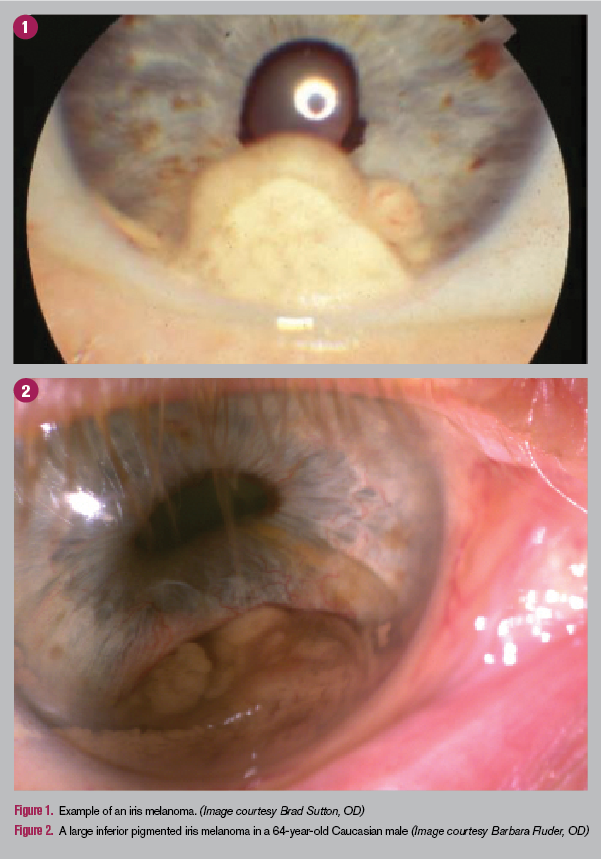

Table 1: Ocular complications observed after treatment
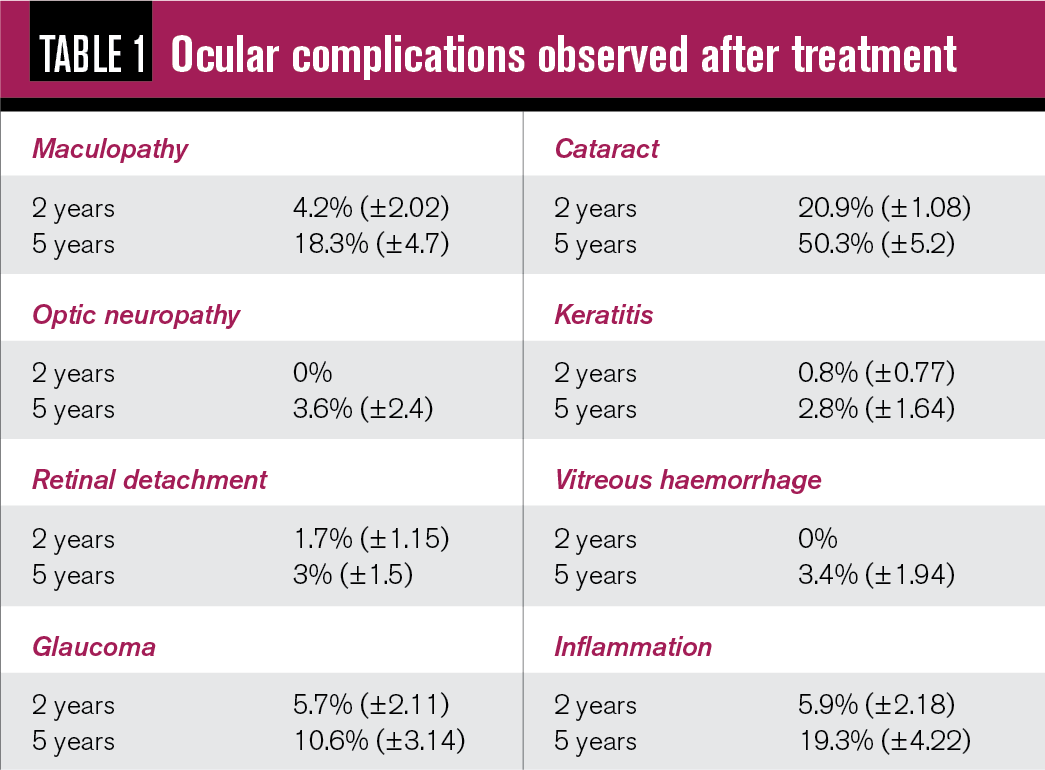
Table 1: Ocular complications observed after treatment

Table 1: Ocular complications observed after treatment

Table 1: Ocular complications observed after treatment

Table 1: Ocular complications observed after treatment

Table 1: Ocular complications observed after treatment

A number of known identifiers of poor prognosis for uveal melanoma are available that can determine patients at a high risk for developing metastasis and who may benefit from targeted treatment.
Although uveal melanomas are rare, they are the most common primary malignancy of the eye in adults.1 For most melanomas, approximately 90 percent arise from the choroid and ciliary body. Only about 10 percent arise from the iris (see Figure 1).1
Treatment options depend on numerous factors, including the size and location of the tumor, the patient’s age and overall health, as well as his life expectancy. These tumors generally develop in older individuals.
Prognosis depends on the cell type of the tumor, size, location, the amount of ciliary body involvement, and evidence of extraocular involvement.
Related: How to identify ocular cancer
Regarding cell type, tumors consisting of spindle-A cells have the best prognosis, and epithelioid cell tumors have the worst prognosis.2 There can also be a combination of the two: a “mixed-cell” type.3
Iris melanomas arise from melanocytes of the iris stroma. They tend to occur more frequently in light-skinned individuals with blue irides.3 About 80 percent of iris melanomas are located in the inferior quadrant of the iris. Tumors can present as circumscribed or diffuse, lobular or flat, with variable pigmentation ranging from deeply pigmented to amelanotic.
Secondary findings may include ectropion iridis, secondary glaucoma, cataract, and prominent vasculature. Patients may be asymptomatic or present with large tumors causing vision loss, visual field defects, spontaneous hyphema, corneal edema, and band keratopathy due to corneal compression. Patients presenting with diffuse melanomas often have hyperchromic heterochromia and secondary glaucoma, and these tumors are more likely to produce metastatic disease.4
Related: Look at the retina in a different way
Case report
A 64-year-old Caucasian male presented to the local retinal specialist with a subconjunctival hemorrhage, hyphema, and vitreous hemorrhage in July 2018. The patient reported noticing decreased vision in his right eye after an episode of vomiting and coughing. He had also been experiencing ocular discomfort intermittently for several months.
The patient was already prescribed timolol (Timoptic, Bausch + Lomb) twice daily, Pred Forte (prednisolone acetate, Allergan) four times daily, and atropine once daily from an ophthalmologist for unknown reasons. The patient has a history of blood clots and was being treated for hypertension, diabetes mellitus, and cardiovascular disease, which required stent surgery placement.
Visual acuity was hand motion at one foot OD and 20/50+2 OS. Intraocular pressures (IOP) were 16 mm Hg OD and 9 mm Hg OS. A B scan was performed to confirm the vitreous hemorrhage and to rule out retinal detachment and tumor. A spontaneous hyphema of unknown etiology was noted, and no notation of an iris melanoma was made. Cataracts were noted as well.
Related: What you don't know about choroidal melanoma
Follow-up
At a one-week follow-up visit with the retinal specialist, records show a resolving subconjunctival hemorrhage, hyphema, and vitreous hemorrhage. Pain was still noted and vision was hand motion at one foot OD, 20/50 OS. IOPs were 15 mm Hg and 16 mm Hg, respectively. A notation was again made that these findings seem to be of unknown etiology.
The patient was referred to the University of Illinois at Chicago due to the unclear diagnosis. The patient failed to appear at the University of Chicago in July 2018. He presented to my office on March 28, 2019, with a red eye, decreased vision, and pain off and on, and was told he has blood in his eye.
The patient had restarted his Pred Forte OD once daily. Visual acuity was counting fingers at six feet OD using eccentric fixation and 20/40 OS. IOPs were 18 mm Hg and 10 mm Hg, respectively. Corectopia was present. Confrontational visual field showed a superior defect. The conjunctiva had a Grade One injection. Cornea was clear. There was no hyphema noted; however, a large inferior pigmented iris melanoma was noted (Figure 2).
The lesion measured 12 mm across the base with a thickness of 5.5 mm. Tumor and iris vascularity were noted. A cataract was present as well. The fundus evaluation was limited due to poor pupil dilation and cataract. A photo of the tumor was taken and shown to the patient along with an explanation of the severity of the condition.
Related: Identifying malignant eyelid tumors
The patient was referred to a retinal specialist at the University of Illinois at Chicago, who saw the patient on April 16, 2019, and confirmed the diagnosis of malignant melanoma of the iris with posterior extension of the lesion into the periphery on the inferior quadrant. No evidence of extraocular extension was noted. A systemic assessment was performed and no metastatic disease was present.
Treatment strategy
Treatment options for this condition include brachytherapy, surgical resection, or enucleation surgery. This patient’s tumor has far too large a base to warrant surgical resection. The patient opted for iodine-125 brachytherapy.
In May 2019, treatment was initiated with a 16-mm plaque to a treatment depth of 5.5 mm. The patient was placed on Pred Forte, atropine, and ofloxacin (Ocuflox, Allergan). There is no documentation on how long the plaque therapy lasted.
Related: How I am embracing the medical model in optometry
The patient was seen for follow-up in June 2019 and reported moderate discomfort. Visual acuity was 4/200 OD. The tumor appeared stable and unchanged in size and appearance. The ocular irritation reported by the patient was due to the radioactive plaque placed over the corneal surface. Artificial tears were added to aid with discomfort, and postop drops were continued.
The patient was seen again in July 2019, and vision was 1/200 OD. The vision remained compromised due to cataract formation and a small degree of corneal edema. The tumor remained unchanged in size and appearance both anteriorly and posteriorly prior to brachytherapy treatment.
The patient will be seen again in January 2020 to reassess and discuss the possibility of cataract surgery.
According to the retinal specialist, the majority of primary uveal melanomas are treated with brachytherapy. If the cancer has spread from the lung or breast to the eye, it is generally treated with external beam radiation because these tumors are more radiosensitive. Brachytherapy demonstrates about an 80 to 90 percent success rate in terms of tumor containment.2
Related: Anterior segment imaging may have saved a life
Retrospective study
A retrospective study for patients treated between January 1990 and December 2000 by iodine-125 plaque brachytherapy for uveal melanoma anterior to the equator has been conducted.5
The tumors were 18 mm or less in diameter. Local or general anesthetic was used for plaque insertion. The diameter of the tumor was determined and was covered by the plaque, allowing for a circumferential safety margin of 2 mm. Plaque diameters used were 12, 14, 16, 18, and 20 mm. The application time was calculated to deliver a total dose of 90 Gray (Gy) to the tumor apex. The time varied in relation to the tumor thickness, plaque diameter, and iodine grain radioactivity.5
Related: Prevention, artificial intelligence, and the future of optometry
Follow-up visits included at one month and every six months, including intermediary visits with the patient’s local ophthalmologist. These visits included visual acuity, systemic assessments for complications associated with irradiation, cataract evaluation, and checking for increased IOP, keratitis or dry eye, and intraocular inflammation. An internal evaluation was done to assess for maculopathy and optic neuropathy.5
The goal of the study was to evaluate the efficacy of the treatment of local and systemic tumor control, along with any associated complications with lesions anterior to the equator. The study included 136 patients (45 men, 91 women) with a median age of 65 and a mean age of 61, and a median follow-up of 62 months. A total of 67 of the tumors were in the right eye, 69 in the left. The median dose delivered to the tumor apex was 101 Gy, and the mean dose was 112 Gy. The mean length of the dose delivered was six days. The mean visual acuity at the time of diagnosis was 20/50.
At the end of follow-up care, 121 patients (89 percent) were alive and 15 (11 percent) had died. Five patients died due to metastatic melanoma, a second cancer for one patient, intercurrent disease in four patients, and an unknown cause of death in five patients. The overall survival rate was 93.8 percent at two years and 88.3 percent at five years. The metastasis-free interval was 98.3 percent at two years and 96 percent at five years. Mean visual acuity at the last follow-up was 20/40. Ocular complications included cataract, glaucoma, keratitis, inflammation, retinal detachment, maculopathy and optic neuropathy (Table 1).
Related: New app detects pediatric leukocoria
Risk factors for overall survival were age >65 years and initial tumor size >4 mm. Ciliary body involvement did not appear to be a significant risk factor. Risk factors for cataract formation were patient’s age, gender, and tumor diameter. Risk factors for glaucoma were only gender, and factors for intraocular inflammation were tumor thickness and ciliary body involvement.5
The Collaborative Ocular Melanoma Study
In September 1985, funding was granted by the National Eye Institute to develop The Collaborative Ocular Melanoma Study (COMS). This was a “multicenter investigation designed to evaluate therapeutic interventions for patients who have choroidal melanoma.”6
The COMS reported an overall 5-year survival rate of 82 percent with brachytherapy while showing no significant difference compared to patients treated with enucleation.
Related: ODs must examine more than just eyes
Indicators of prognosis
In addition to clinical features, histologic, cytogenetic, and gene expression markers can now help estimate the prognosis of uveal melanoma. This additional information can identify those patients at a high risk for developing metastasis and who may benefit from targeted treatment.7
Tumor sample for testing is obtained from enucleation surgery or intraoperative fine-needle aspiration biopsy. Tumor features presenting with the following are indicative of a poor prognosis:
- Epithelioid cells, high mitotic activity
- High values of mean diameter of the 10 largest nucleoli (MLN)
- High microvascular density
- Extravascular matrix patterns
- Tumor-infiltrating lymphocytes
- Tumor-infiltrating macrophages
- High expression of insulin-like growth factor-1 receptor (IGF-1R)
- High expression of human leukocytic antigen class 1 and 2
Genetic factors-including monosomy 3, 1p loss, 6q loss, and 8q gain-are also indicative of poor prognosis. Regarding cell type, a study of 2,652 enucleated eyes with uveal melanoma, the 15-year mortality for spindle-A tumor was 19 percent, spindle B was 26 percent, mixed spindle B and epithelioid was 59 percent, and epithelioid was 72 percent. Spindle-cell melanomas have the best prognosis followed by mixed cells, and epithelioid have the worse prognosis.7
Tumors with high cellular proliferation or mitosis have a poor prognosis compared to tumor cells with less mitotic activity.7 Large MLN is seen in tumors with epithelioid cells and is a poor prognosis indicator. Microvascular density (MVD) is a quantitative measurement of tumor vascularity and, along with a large MLN, can influence a poor prognosis.7
Related: Propolis may help treat ocular disease
Microvascular patterns can be an indicator of prognosis as well. The presence of at least one closed vascular loop in a uveal melanoma is associated with the presence of epithelioid cells and is the most significant vascular pattern associated with mortality from malignant melanoma.7
Increased tumor-infiltrating lymphocytes and macrophages are also indicators of poor prognosis. These tumors also present with epithelioid cells and have an increased MVD. Increased lymphocytes in tumor cells result in increased production of inflammatory mediators, generating a tumor-promoting inflammatory microenvironment. M2 phenotype macrophages promote phagocytic activity, tissue remodeling, tumor progression, and angiogenesis.7
Related: Drug offers hope in treating ocular melanoma
Increased IGF-1R levels in tumors significantly indicates a poor prognosis. IGF-1R is mainly produced in the liver, the most common site. IGF-1R blockage may be a treatment option for metastatic disease, and serum IGF-1R levels may be a biomarker for metastatic uveal melanoma.7
Regarding cytogenetic features, a complete loss of one copy of chromosome 3 (monosomy 3), seems to be the most common and most important factor. It is associated with other factors, including large tumor diameter, ciliary body tumor location, epithelioid cell type, high mitotic rate, vascular loops, and extraocular extension. The tumor suppressor gene BRCA1-associated protein 1 has been mapped to chromosome 3p21.1 and has been associated with metastatic uveal melanoma.7
Early detection of uveal melanoma when the tumor is small and at the least risk of metastasis is the most effective treatment. In addition to clinical assessment, histologic, cytogenetic, and transcription markers are also available to estimate the prognosis of uveal melanoma.
More by Dr. Fluder: Offer options to your cataract patients
References:
1. Harbour JW. An update on uveal melanoma. Rev Ophthalmology. Available at: https://www.reviewofophthalmology.com/article/an-update-on-uveal-melanoma. Accessed 2/18/20.
2. Stephenson M. Better options emerging in ocular oncology. Rev Ophthalmology. Available at: https://www.reviewofophthalmology.com/article/better-options-emerging-in-ocular-oncology. Accessed 2/18/20.
3. Manhattan Eye, Ear, and Throat Hospital, Department of Ophthalmology. Color Atlas of Ophthalmology: The Manhattan Eye, Ear, and Throat Hospital Pocket Guide. Eds: Mandava S, Sweeney T, Guyer D. Pp. 329-330. New York, New York: Thieme. 1999.
4. Shields JA, Shields C. Tumors of the Uveal Tract. In: Duane’s Atlas of Ophthalmology: Vol. 4 (Tasman W, Jaeger EA, Eds.) Philadelphia: Lippincott Williams & Wilkins. 2009.
5. Lumbroso-Le Rouic L, Charif Chefchaouni M, Levy C, Plancher C, Dendale R, Asselain B, Solignac S, Mazal A, Desjardins L. 125I plaque brachytherapy for anterior uveal