- Therapeutic Cataract & Refractive
- Lens Technology
- Glasses
- Ptosis
- AMD
- COVID-19
- DME
- Ocular Surface Disease
- Optic Relief
- Geographic Atrophy
- Cornea
- Conjunctivitis
- LASIK
- Myopia
- Presbyopia
- Allergy
- Nutrition
- Pediatrics
- Retina
- Cataract
- Contact Lenses
- Lid and Lash
- Dry Eye
- Glaucoma
- Refractive Surgery
- Comanagement
- Blepharitis
- OCT
- Patient Care
- Diabetic Eye Disease
- Technology
How to treat dry eye in the pediatric and young adult population
Always look for dry eye in patients of all ages
Figure 1. Image courtesy Scott Schachter, OD
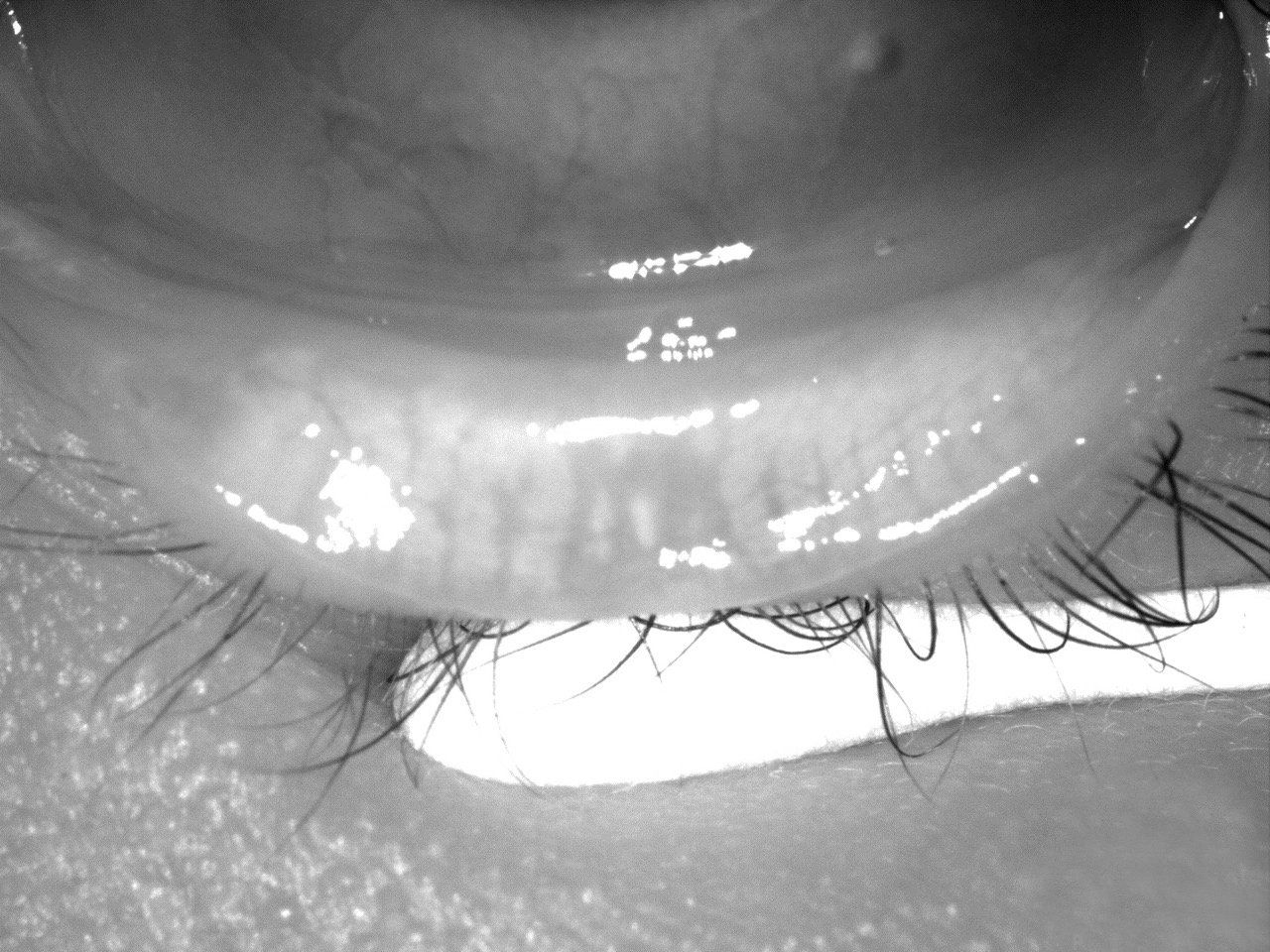

When ODs think about dry eye, they quickly associate classic demographics: Over-40 menopausal female patients taking a high number of medications or individuals with autoimmune disease. But are ODs overlooking a younger, seemingly healthy demographic?
Optometrists are diagnosing dry eye more than ever before. Whether that is due to the culture’s screen-saturated lifestyles, an increased awareness about dry eye-or more likely-a combination of both, I have observed an increase in dry eye among my younger patients in their late teens and twenties. These are people who we rarely saw just a few years ago-even in my practice at an advanced dry eye treatment center.
Related: The most important objective dry eye test is TBUT with fluroescein, ODs say
Diagnosing dry eye in young patients
Journal articles and medical conferences have certainly increased awareness that dry eye is a pathology that can affect patients of all ages, although it is rare to see dry eye in healthy pediatric patients. ODs have made progress in monitoring the vision and health components of children at birth, but optometric efforts need to expand in scope to include the anterior segment and to be encouraging as children become more independent in caring for themselves.
Early in my career, I fell under the same pitfalls that I suspect many of my colleagues also did: I superficially treated dry eye symptoms, particularly in adolescent and young adult patients. As my own awareness and understanding of the chronic nature of dry eye increased, my propensity to be more aggressive in treating it with the younger patient population grew as well.
Related: Blog: Why dry eye?
Ask the right questions
Asking the right questions to get the right answers is essential to helping younger patients articulate their symptoms. Young children simply have not developed the awareness or vocabulary to tell us how they feel, and tweens and teens may not understand that they can discuss anything outside of glasses and contacts with their optometrist.
General questions may be enough to get the conversation going, such as:
• Do your eyes feel dry?
• Do your eyes get red?
• Do you rub your eyes a lot?
• How much time do you spend looking at screens?
Ultimately, questions should shed light on the effect of accommodation to the visual system.
For pediatric patients, the questions should extend to the parents. A personal or family history of atopy (particularly with an element of eczema), rheumatological conditions, and autoimmune disease are triggers to ask about.
Related: Know how to care for pediatric patients diagnosed with Down syndrome
Diagnostic testing
Regardless of the patients’ age, looking for dry eye signs from a clinical perspective appears much the same from behind the microscope.
In my experience, children and teens are generally tolerant of quick and painless testing, such as osmolarity or meibography, so go ahead and run these tests.
The screen factor
Everyone has heard that environment is to blame for virtually everything, and dry eye is likely just one more negative environmental manifestation-specifically the exponential increase of screen time for Americans of every age.

Starting in infancy, children gravitate to the glowing screen in their parents’ hands; school-aged children are required to study and complete assignments online; and adults shop, socialize, and work using their beloved screens. Add in entertainment, and the hours people spend in front of a screen are staggering. It is not a surprise that current research suggest that screen time may play a significant role in dry eye.1Related: How to recognize and manage digital eye strain
While it is easy to say that adults should monitor and limit screen time for children (there’s an app for that!), ODs must also accept that screens are a necessary part of the world they live in. Realistically, ODs are unlikely to convince their patients to significantly reduce their use of screens; however, educating them on the possible effects of screen time, such as reduced or incomplete blinking, is a great place to start.
I like to teach the 20-20-20 rule: Every 20 minutes, screen users should look up for 20 seconds and focus on an object at least 20 feet away.
In addition, we can remind patients to make a conscious effort to blink completely and simply open and close their eyes throughout the day.
Related: Why my passion for pediatric exams stays personal
Treating young patients

The multifactorial nature of dry eye requires consideration of inflammatory and obstructive components, the impact of blepharitis, and the patients’ biofilm.
Foundational treatment begins with good lid hygiene, and young children can benefit from learning and establishing proper hygiene routines with gentle products. Any patient presenting with blepharitis should establish a regimen with a product such as HypoChrlo hypochlorous lid wipes (OCuSOFT) and perhaps warm compresses such as a Bruder mask.
Related: Treating blepharitis in the pediatric population
Additionally, I often prescribe the use of artificial tears, such as Refresh Relieva (Allergan). Drop instillation tends to provoke a visceral response in patients of every age, and especially young patients. Therefore, it is very important to avoid creating a negative experience for both parents and child because parent don’t want to wrestle their children at every dosing. A positive association means compliance is far more likely.
I recommend pediatric patients lay down flat, get comfortable, and close their eyes like they are sleeping. With the eyes closed, drop the medication right at the lateral canthus, then ask patients to open the eyes to allow the tear to roll in. This is a nonthreatening process, and children usually feel immediate soothing effects and develop a positive association with drop instillation.
The nutrition factor
As an optometrist, I approach nutrition from a reinforcing perspective. I keep the discussion simple and conversational by asking my patients if they think they have a perfect diet (this usually gets a laugh from parents).
I then explain that nobody can have a perfect diet, and that some of the nutrients we need are not consumed in the typical diet, such as plant-based black currant seed oil. However, we can provide our body with needed nutrients that will potentially manage the symptoms and prevent irreversible damage with high-quality supplements, such as HydroEye (ScienceBased Health) which has demonstrated efficacy in improving dry eye symptoms, EyePromise EZ Tears (ZeaVision), BioTears (BioSyntrx), and others.2,3Related: ODs reach for artificial tears first to treat dry eye
Supplemental omega fatty acids have been shown to reduce inflammation and improve the overall quality of tears. There is a growing body of evidence that shows that the omega-6 gamma-linolenic acid (GLA) is highly effective for treating patients with dry eye.4 When combined with omega-3 fatty acids, such as eicosapentaenoic acid (EPA), they decrease pro-inflammatory arachidonic acid and prostaglandin E2.5,6
A randomized, placebo-controlled study shows that nutritional supplements containing EPA and GLA reduce inflammatory biomarkers, improve corneal surface smoothness, and improves symptoms of dry eye.2
Although swallowing a pill may be difficult for very young patients, it is quite feasible for children in their tweens and teens. In addition, I have found that the young adult population is generally open to and even seeking natural methods for treating pathology.
By the time children are able to swallow a supplement, they have usually reached the size of a small adult, so I keep the dosing as recommended by the manufacturer. While not all patients immediately jump on board with nutraceuticals, at least they are made aware that there is a nutrition-based approach to treating dry eye if they wish to pursue it in the future.
Related: Omega-3s no better than placebo for dry eye
Pearls and recommendationsdry eye is a chronic and progressive disease that can eventually cause corneal damage, discomfort, and visual impairment.7 Ask questions and review personal and familial history for known dry eye triggers. Always look for dry eye in patients of all ages, even if you are not expecting it to be present. The sooner ODs can identify and treat the disease, the better for young patients.
Do not be averse to treating pediatric patients and allow them to take ownership of their health. Talk directly to them with the parent overhearing the conversation versus working around the child and going straight to the parent. Explain and show children how to wash around their eyes, apply lid solutions, and to be mindful to close their eyes while washing their faces. Set up pediatric patients (and their parents) to have a positive treatment experience, and consequently better compliance, by using proper drop instillation techniques and gentle products.
Be willing to accept rejection. Sometimes as eyecare providers, ODs are concerned that their patients will not agree to do what they recommend, but ODs still need to have these conversations and provide families with education about the disease. Eventually, they may circle back around and return for treatment.
A “no” to treatment does not mean “never.”
Read more by Dr. Hauser
Dr. Hauser is the founder and senior consultant for Signal Ophthalmic Consulting and founder and CEO of DryEyeCoach.com. She serves as an advisory board member for TearLab and Paragon BioTeck. She consults or speaks for Johson & Johnson Vision, Shire, Lumenis, Allergan, Alcon, Bruder Medical, BioTissue, Sight Sciences, Eyevance, Kala, Sun Pharma, BlephEx, ScienceBased Health, Oculus, and Bausch + Lomb. In her free time she likes to scout out espresso spots and hang out with her three kids.
whauser@sigmalophthalmic.com
References:
1. Moon JH, Kim KW, Moon NJ. Smartphone use is a risk factor for pediatric dry eye disease according to region and age: a case control study. BMC Ophthalmol. 2016 Oct 28;16(1):188.
2. Sheppard, JD, Singh R, McClellan A, Weikert MP, Scoper SV, Joly TJ, Whitley WO, Kakkar E, Pflugfelder SC. Long-term Supplementation With n-6 and n-3 PUFAs Improves Moderate-to-Severe Keratoconjunctivitis Sicca: A Randomized Double-Blind Clinical Trial. Cornea. 2013 Oct;32(10):1297-304.
3. Oleñik A, Jiménez-Alfaro I, Alejandre-Alba N, Mahillo-Fernández I. A randomized, double-masked study to evaluate the effect of omega-3 fatty acids supplementation in meibomian gland dysfunction. Clin Interv Aging. 2013;8:1133-1138.
4. Creuzot-Garcher C, Baudouin C, Labetoulle M, Pisella PJ, Mouriaux F, Meddeb-Ouertani A, El Matri L, Khairallah M, Brignole-Baudouin F. [Efficacy assessment of Nurtilarm, a per os omega-3 and omega-6 PUFA dietary formulation versus placebo in patients with bilateral treated moderate dry eye syndrome.] J Fr Ophtalmol. 2011 Sep;34(7):448-55.
5. Barham JB, Edens MS, Fonteh AN, Johnson MM, Easter L, Chilton FH. Addition of eicosapentainoic acid to gamma-linolenic acid-supplemented diets prevents serum arachidonic acid accumulation in humans. J Nutr. 2000 Aug;130(8):1925-1931.
6. Viau S, Leclère L, Buteau B, et al. Polyunsaturated fatty acids induce modification in the lipid composition and the prostaglandin production of the conjunctival epithelium cells. Graefes Arch Clin Exp Ophthalmol. 2012 Feb;250(2):211-222.
7. National Eye Institute. Facts About the Cornea and Corneal Disease. Available at: https://nei.nih.gov/health/cornealdisease. Accessed 7/30/19.

