Case report: Refractory pseudophakic cystoid macular edema during an exacerbation of scleroderma
It is important that clinicians are prepared with alternative methods for patients experiencing refractory CME after failed improvement with the agents that are most frequently used.
Pseudophakic cystoid macular edema (CME) is a known possible complication associated with cataract extraction surgery.1 Medical therapy for pseudophakic CME typically includes nonsteroidal anti-inflammatory drugs, steroids, carbonic anhydrase inhibitors, anti-VEGF agents, or surgical treatment such as laser photocoagulation.2 As newer agents, anti-VEGF injections such as bevacizumab (Avastin; Genentech) have displayed effectiveness and are well tolerated in patients with refractory pseudophakic CME, with significant improvement in best corrected visual acuity and decrease in macular thickness via optical coherence tomography (OCT) at 12 months.3
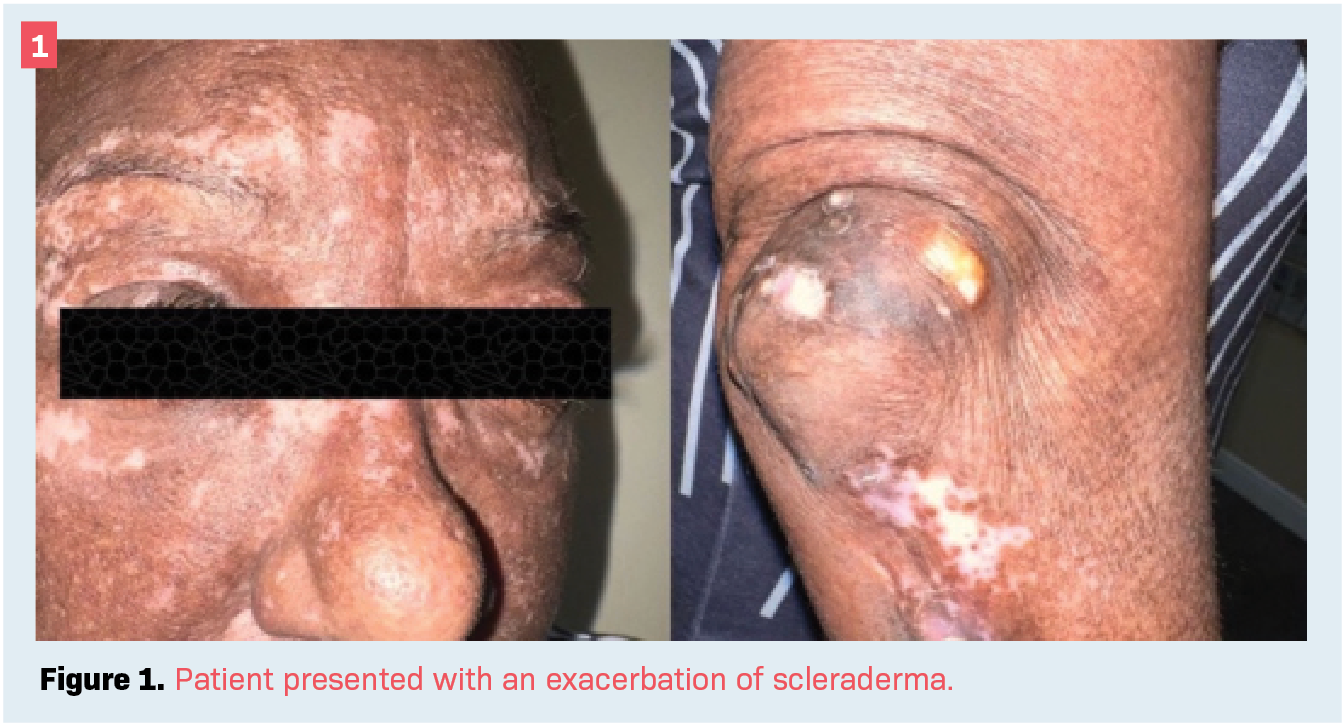
Although there has been improvement with the use of anti-VEGF injections for some patients, we sought a method for improvement in a patient with exacerbation of scleroderma (Figure 1). She continued to exhibit no relief in symptoms despite multiple bevacizumab injections. Scleroderma involves fibrosis of the skin and internal organs due to autoimmunity and vasculopathy.4 Fibroblast dysfunction and increased deposition of extracellular matrix, tissue hypoxia, and immune response are characteristic of scleroderma pathology. Scleroderma has been linked to ocular manifestations, including dry eye disease and inflammatory conditions such as uveitis, episcleritis, and peripheral ulcerative keratitis.5
Patients with scleroderma typically exhibit alterations in biomarkers, including elevated levels of serum IL-6.6-8 Elevated intraocular levels of IL-6 have been linked to anti-VEGF resistance in patients with age-related macular degeneration, a finding which has led us to question whether elevated levels of IL-6 may also contribute to anti-VEGF resistance in patients with scleroderma.9 Such a finding may suggest a need for alternative options in patients experiencing pseudophakic CME with preexisting rheumatic disease and corresponding elevations in proinflammatory cytokines.9
Presentation
A 63-year-old woman presented on April 4, 2022, for a glaucoma follow-up of the left eye. The patient presented 5 months after cataract removal surgery, which had occurred on November 23, 2021, and complained of an inability to see well with her glasses. At the time of presentation, the patient reported an exacerbation of underlying scleroderma.
Medical history
Her complex medical history included hypertension and scleroderma. Ocular history included primary open-angle glaucoma of the left eye, left eye ptosis, vitreous degeneration of the right eye, and pseudophakia of both eyes. Surgical history was significant for cataract extraction with intraocular lens of the left eye in 2018 and cataract extraction with intraocular lens of the right eye in 2021. The patient’s maintenance medication list included daily nifedipine, losartan, atorvastatin, aspirin, and a weekly dose of vitamin D2. Her ocular medication list included twice-daily administration of brimonidine and dorzolamide/timolol for management of glaucoma in her left eye. At the time of presentation, she was taking 4 mg methylprednisolone (Medrol Dosepak) in addition to a 7-day course of clindamycin therapy to manage an exacerbation of scleroderma. She had never smoked and did not drink alcohol.
Work-up, diagnosis, and treatment
Prior to the presence of pseudophakic CME, the patient underwent a cataract extraction with insertion of intraocular lens of the right eye in November 2021. Visual acuity of the right eye prior to surgery was 20/100. The postoperative topical regimen for week 1 consisted of prednisolone (Pred-Forte), diclofenac, and ciprofloxacin, which were to be used 4 times daily in the right eye. The topical regimen for weeks 2 through 4 consisted of prednisolone and diclofenac, which were to be administered in the right eye twice daily.
At the 7-day postoperative visit, visual acuity of the right eye was 20/20. Three weeks after surgery, the patient returned for a follow-up appointment and had a right eye visual acuity of 20/40. The first OCT of the macula of the right eye was performed 3 weeks after cataract surgery of the right eye. Four weeks after surgery, the patient’s visual acuity of the right eye was 20/50 and the patient received a diagnosis of iridocyclitis. She was instructed to resume therapy with prednisolone 4 times daily in the right eye. The patient was then lost to follow-up for the next 4 months and returned with symptoms of pseudophakic CME on April 20, 2022.
Timeline of disease progression
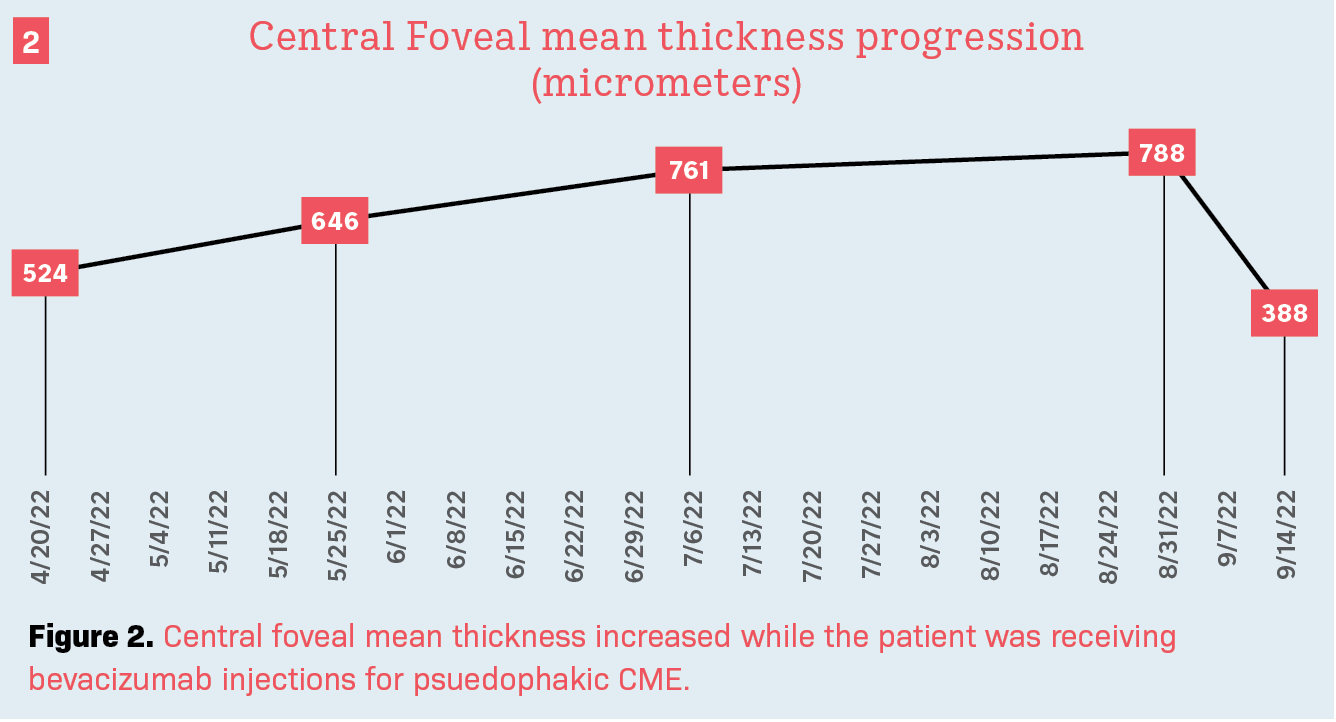
April 20, 2022: Visual acuity on Snellen scale of right eye was 20/50. Applanation of both eyes was 14 mmHg. Pupils were PERRLA. Vitreous of the right eye displayed a prominent Weiss ring with posterior vitreous detachment. Retinal exam via OCT scan of right eye displayed manifestation of CME. The central subfoveal mean thickness measured 524 μm (Figures 2 & 3). Bevacizumab injection was planned at this visit. Topical steroids and nonsteroidal anti-inflammatory drugs were not reinstituted because of the severity of disease upon her return after loss to follow-up. Acetazolamide (Diamox; Heritage Pharmaceuticals) was not prescribed because of a potential major drug interaction with her daily use of aspirin. Triamcinolone (Kenalog; Bristol-Myers Squibb) was not offered as an option because of risk of glaucoma in this patient.
April 27, 2022: Bevacizumab injection (1.25 mg/0.05 mL) was performed after sterile preparation with povidone iodine, tetracaine, and lidocaine gel. Erythromycin ointment was placed in the cul-de-sac, and the patient was given a follow-up appointment.
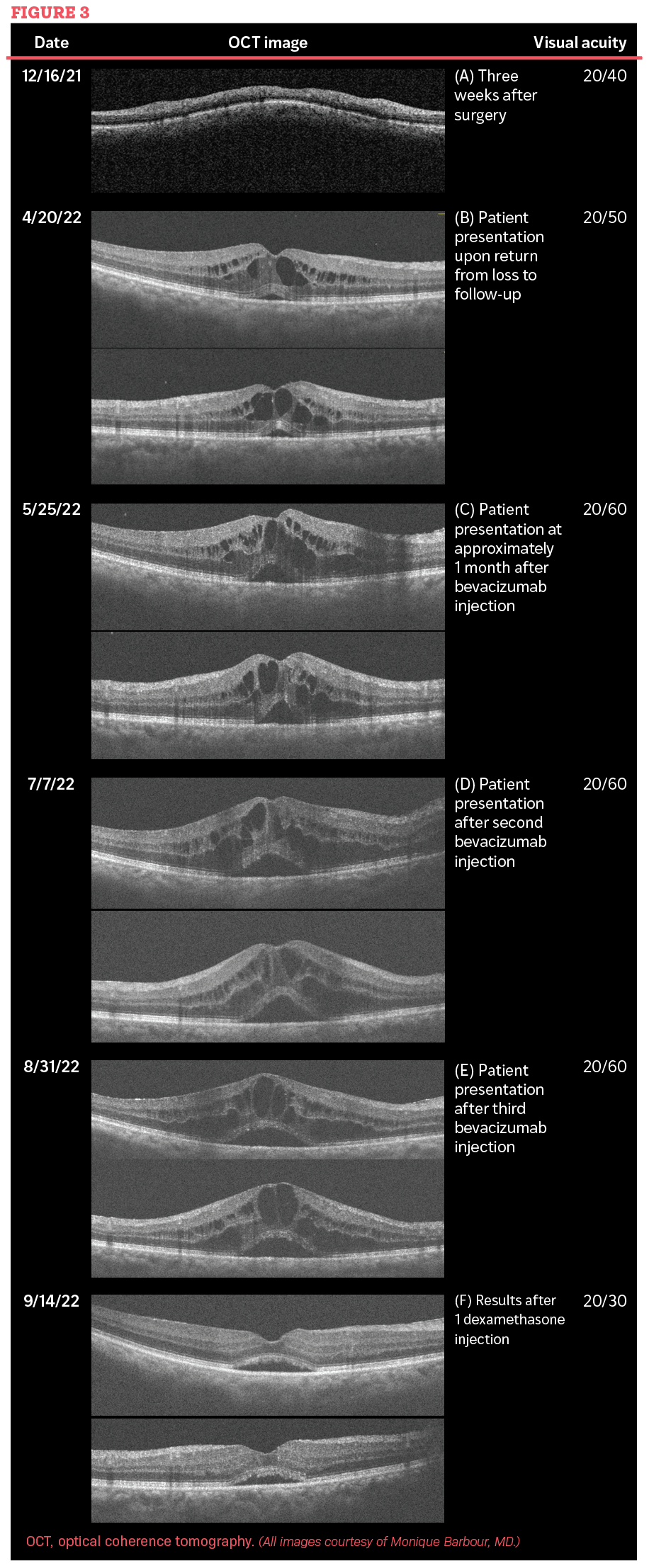
May 25, 2022: The patient returned with a chief complaint of constant black spots in the vision of her right eye. Symptoms were noted to occur when the patient was located both indoors and outdoors. The complaint was associated with blurry vision and no eye pain. Results of OCT reflected an increased central foveal mean to 646 μm. Visual acuity was 20/60.
June 1, 2022: Bevacizumab injection (1.25 mg/0.05 mL) was repeated.
July 7, 2022: The patient returned with a chief complaint of no relief in her right eye and noticed that her vision had become worse since the last injection. Central foveal mean thickness displayed an increased value of 761 μm. Visual acuity was 20/60. Bevacizumab injection was repeated.
August 31, 2022: The central foveal mean thickness was measured at 788 μm. Visual acuity was 20/60. Patient’s therapy was switched from bevacizumab to the dexamethasone 0.7-mg implant (Ozurdex), which was administered in the vitreous of the right eye.
September 14, 2022: The patient returned for a follow-up and reported that her affected eye was now doing well. Two weeks following a single insertion of dexamethasone displayed an improvement in central foveal thickness from 788 μm to 388 μm. Visual acuity was 20/30.
The patient maintained an improvement in symptoms at follow-up appointments on October 26, 2022, and November 2, 2022. The original expected outcome of pseudophakic CME in this case was an improvement in symptoms after administration of anti-VEGF treatment via bevacizumab injection. The actual outcome was a case of pseudophakic CME which was refractory to treatment with 3 administrations of bevacizumab at approximately 30 to 40 days apart.
Discussion
Dexamethasone is currently FDA approved to manage macular edema following branch retinal vein occlusion or central retinal vein occlusion, diabetic macular edema in the general population, and noninfectious posterior segment uveitis.10 After the observed results of our case report, dexamethasone might also be useful as off-label treatment for patients with refractory pseudophakic CME after failed improvement via use of anti-VEGF agents. Similar results were reported from Meyer et al,11 who concluded that the use of the dexamethasone 0.7-mg implant was beneficial in the management of Irvine-Gass syndrome after failed improvement from dexamethasone 0.4-mg injections.
Although most cases of CME resolve spontaneously, those who are affected may experience clinically significant decrease in visual acuity.2 It is important that we, as clinicians, are prepared with alternative methods for patients experiencing refractory CME after failed improvement with the agents that are most frequently used. In our society with extended life spans, cataract cases and associated cataract removal surgeries will continue to rise because the prevalence of the condition increases with age.12 More surgical cases will likely lead to an increased population of patients experiencing pseudophakic CME. Our patient’s vision improved from 20/50 to 20/30 in her right eye from initial presentation to most recent follow-up visit. Dexamethasone should be reviewed as an option to treat those who have not been responsive to other treatment methods as we aim to provide the best care for our patients that we can.
References
Jacobs DS. Cataract in adults. UptoDate. Accessed April 26, 2023. https://www.uptodate.com/contents/cataract-in-adults
Rotsos TG, Moschos MM. Cystoid macular edema. Clin Ophthalmol. 2008;2(4):919-930. doi:10.2147/opth.s4033
Arevalo JF, Maia M, Garcia-Amaris RA, et al; Pan-American Collaborative Retina Study Group. Intravitreal bevacizumab for refractory pseudophakic cystoid macular edema: the Pan-American Collaborative Retina Study Group results. Ophthalmology. 2009;116(8):1481-1487.e1. doi:10.1016/j.ophtha.2009.04.006
Gilbane AJ, Denton CP, Holmes AM. Scleroderma pathogenesis: a pivotal role for fibroblasts as effector cells. Arthritis Res Ther. 2013;15(3):215. doi:10.1186/ar4230
Gomes BAF, Santhiago MR, Magalhães P, Kara-Junior N, Azevedo MNL, Moraes HV Jr. Ocular findings in patients with systemic sclerosis. Clinics (Sao Paulo). 2011;66(3):379-385. doi:10.1590/s1807-59322011000300003
Kawaguchi Y. Contribution of interleukin-6 to the pathogenesis of systemic sclerosis. J Scleroderma Relat Disord. 2017;2(suppl 2):S6-S12. doi:10.5301/jsrd.5000258
Maleki A. Scleroderma. In: Foster CS, Anesi SD, Chang PY, eds. 2021. Uveitis. Springer, Cham; 2021:15-19. https://doi.org/10.1007/978-3-030-52974-1_4
Karkhur S, Hasanreisoglu M, Vigil E, et al. Interleukin-6 inhibition in the management of non-infectious uveitis and beyond. J Ophthalmic Inflamm Infect. 2019;9(1):17. doi:10.1186/s12348-019-0182-y
Correa F, Jacobson R, Prasad N, et al. Development of novel bispecific anti-inflammatory and anti-angiogenic therapy for the treatment of both retinal vascular and inflammatory diseases. Invest Ophthalmol Vis Sci.2019;60(9):5396.
FDA approves revised indication for Ozurdex for diabetic macular edema. The American Society of Retina Specialists. Updated September 29, 2014. Accessed November 21, 2022. https://www.asrs.org/clinical/clinical-updates/368/FDA-Approves-Revised-Indication-for-Ozurdex-for-Diabetic-Macular-Edema
Meyer LM, Schönfeld CL. Cystoid macular edema after complicated cataract surgery resolved by an intravitreal dexamethasone 0.7-mg implant. Case Rep Ophthalmol. 2011;2(3):319-322. doi:10.1159/000332424
Hashemi H, Pakzad R, Yekta A, et al. Global and regional prevalence of age-related cataract: a comprehensive systematic review and meta-analysis. Eye (Lond). 2020;34(8):1357-1370. doi:10.1038/s41433-020-0806-3

Newsletter
Want more insights like this? Subscribe to Optometry Times and get clinical pearls and practice tips delivered straight to your inbox.