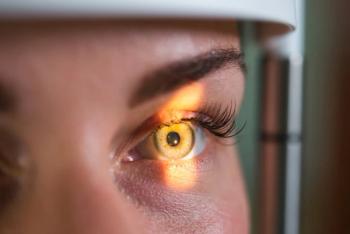
How we manage acute conjunctivitis
To more efficiently manage time, a New York-based practice has increased the role of technicians to include taking a role in managing acute conjunctivitis. Implementing a dedicated red-eye protocol calls on technicians to screen patients and administer the AdenoPlus test. The results are available before the doctor enters the room.
At the Cornea Service and Refractive Surgery Center in New York, my colleagues and I approach the management of acute conjunctivitis as a team effort. We have adopted a strategy that is beneficial for our patients and doctors and easy for our technicians to follow, with minimal training.
Dr. AsbellIn an effort to efficiently manage time, our practice has increased the role technicians play to include managing acute conjunctivitis. By implementing a red-eye protocol dedicated to effective management of acute conjunctivitis, our technicians are now able to screen patients and perform the AdenoPlus (Nicox Inc.), a rapid, point-of-care test that aids in the differential diagnosis for acute conjunctivitis. Now, if a patient presents with a red eye, a technician initiates the protocol by obtaining the patient’s history, triaging him or her to an exam room as quickly as possible, and administering the AdenoPlus test. The results are available before the doctor enters the room.
The test results have been in line with our clinical diagnostic skills and the results of our macro-biology and virology laboratory. The key advantage of doctors and technicians working together to confirm the presence of adenovirus is ensuring that we do not unnecessarily contaminate the office, other patients, and even staff. The contagious nature of the adenovirus is not new to us; however, its rapid diagnosis is. The technician is able to essentially screen patients to control contagion. We want to protect our patients who are coming in and out of surgery and have more sensitive eyes.
Further, the morbidity associated with the adenovirus is severe conjunctivitis, red eye, swollen lids, pseudomembranes, inflammatory tissues on the surface of the eye, and subepithelial infiltrates in the cornea that can persist. If the test is positive for adenovirus, the technician first puts a flag outside of the room, which alerts the staff that the room has been contaminated. We then communicate to the patient the contagious nature of the virus, that it is likely to spread to the second eye, the serious risk of passing it on to others, and how the patient can limit the spread to others. If the test is negative, then we can explore the possibility of a different viral infection, which typically does not cause such a severe acute conjunctivitis and isn’t as contagious. Giving the patient an accurate diagnosis, either way, allows us to discuss treatment options more intelligently than we could if we did not definitively know the patient’s condition.
Patients respond positively to our method for managing acute conjunctivitis because they leave our office receiving exactly what they came in for: a diagnosis. Uncertainty adds significant stress to anyone with a medical problem. Having a diagnosis and the facts behind it gives patients a sense of security and trust within our practice.
It is important to let patients know with confidence that a diagnosis has been reached because there is no FDA-approved drug for treating adenoviral conjunctivitis. Accordingly, we explain that to patients and discuss steroids as an option, which may help or worsen the infection. We may also consider a topical antiviral, such as ganciclovir (Zirgan; Bausch + Lomb), which is FDA approved for treating ocular herpes infections but is an off-label, non–FDA-approved option for treating ocular adenoviral infections. There is limited data suggesting it may be helpful with adenoviral infections.1-5
If a technician performs the diagnostic test and a viral infection is ruled out, a doctor can then move forward with determining whether the patient has bacterial or allergic conjunctivitis. Nearly all allergic conjunctivitis cases have itchiness as a symptom. If the patient isn’t experiencing itchiness at all, it is unlikely that that he or she has an allergic reaction. Also, patients with allergies generally experience other allergic reactions, such as asthma and skin problems, which suggest they are prone to allergic conjunctivitis. If the patient’s eyelid skin is swollen or has fine wrinkles, that is an indication of an allergic reaction because we don’t typically see wrinkles with a bacterial or viral infection. Signs that a patient has a bacterial infection include a thick discharge vs. a watery discharge, which is common with viral infections. Also, bacterial infections are typically unilateral (in only one eye), whereas viral infections are almost always bilateral (in both eyes).
Medications for bacterial conjunctivitis depend on associated risk factors, such contact lens wear, corneal involvement, or abrasion that could lead to an infection. In this case, we may prescribe fluoroquinolones, which have good broad-spectrum activity. We sometimes prescribe trimethoprim, which has been proven to be effective against methicillin-resistant Staphylococcus aureus (MRSA).6-7
For allergic conjunctivitis, we design the treatment plan based on what type of allergy the patient is dealing with. If the patient is allergic to environmental findings, such as pollen, we prescribe an antihistamine/mast-cell stabilizer. We also prescribe artificial tears as a lubricant to wash out allergens or substances that might be causing the reaction. We suggest that patients store the tears in the refrigerator because the cold temperature can be soothing and decrease itchiness and irritation related to the allergic response. If the patient has erythema and swelling of the lids, he or she may have contact dermatitis. Therefore, it is important that the technician take a careful history from the patient because this also aids in determining the treatment.
Patients respond well to both technicians’ and doctors’ involvement in care and treatment. We recommend implementation of a dedicated red eye protocol for any practice because it improves the standard of care for acute conjunctivitis management.ODT
References
Epstein SP, Fernandez KB, Carter BM, Abdou SA, Gadaria, N, and Asbell, PA. Safety and efficacy of ganciclovir ophthalmic gel for treatment of adenovirus keratoconjunctivitis utilizing cell culture and animal models. Inv Ophthalmol Vis Sci. 2012;(Suppl.)53(4):S6203.
Naesens L, Lenaerts L, Andrei G, Snoeck R, Van Beers D, Holy A, Balzarini J, De Clercq E. Antiadenovirus activities of several classes of nucleoside and nucleotide analogues. Antimicrobial Agents Chemotherapy. 2005; 49(3):1010–1016.
Crumpacker CS. Drug Therapy: Ganciclovir. N. Engl. J. Med. 1996; 335(10):721–729.
Trousdale MD, Goldschmidt PL, Nóbrega R. Activity of ganciclovir against human adenovirus type-5 infection in cell culture and cotton rat eyes. Cornea. 1994; 13(5):435-439.
Tabbara K, Jarade E. Ganciclovir effects in adenoviral keratoconjunctivitis. Invest Ophthalmol Vis Sci. 2001;3111 (suppl); S579.
Asbell PA, Sahm DF, Shaw M, Draghi DC, Brown NP. Increasing prevalence of methicillin resistance in serious ocular infections caused by Staphylococcus aureus in the United States: 2000 to 2005. J Cataract Refract Surg. 2008;34(5):814-818.
Asbell PA, Colby KA, Deng S, McDonnell P, Meisler DM, Raizman MB, Sheppard JD Jr, Sahm DF. Ocular TRUST: Nationwide Antimicrobial Susceptibility Patterns in Ocular Isolates. Am J Ophthalmol. 2008;145(6):951-959.
Take-Home Message
To more efficiently manage time, a New York-based practice has increased the role of technicians to include taking a role in managing acute conjunctivitis. Implementing a dedicated red-eye protocol calls on technicians to screen patients and administer the AdenoPlus test. The results are available before the doctor enters the room.
Time management for managing patient care
By Wanda Hernandez
HernandezThe extent of my role in in a red eye protocol for conjunctivitis lies in its execution.
When the practice first implemented the protocol, it was on a trial basis, and it was managed completely by the our doctors. There had come a point where it was taking too long for our doctors to get around to the patients to administer the diagnostic test. To save time, I started jumping in and administering the diagnostic test. From there, the other technicians followed suit.
Now, on a day-to-day basis, techs are administering this critical part of our practice’s red eye protocol. It takes just seconds to obtain a tear sample from a patient and only 10 minutes before results are available. The learning curve for technicians performing the diagnostic test relates to obtaining enough of a tear sample and, although instructions state to use a dab-and-drag motion in 6 to 8 locations on the lower eyelid to collect a sample, it is important for technicians to realize that the area is sensitive.
Our previous protocol required patients to wait to see the doctor before even being given a diagnosis. Following that interval, patients next had a 3-day wait before receiving lab results to confirm adenoviral conjunctivitis.
Now patients are very grateful to receive more immediate diagnoses and well-rounded treatment. From the practice side, there is a consensus among technicians that we feel more involved in the patient care process and a better sense of job fulfillment because we are executing the test. The protocol is centered on executing the diagnostic test so, essentially, the process is in our hands. While the patient waits to see the doctor, the techs can answer any questions the patient may have. In turn, doctors are able to better manage their time and provide an accurate and directed treatment plan.
Together, we as technicians are helping doctors improve the standard of care for managing acute conjunctivitis.ODT
Newsletter
Want more insights like this? Subscribe to Optometry Times and get clinical pearls and practice tips delivered straight to your inbox.