
Quick diagnosis leads to better outcomes and reduces long-steroid usage.

Quick diagnosis leads to better outcomes and reduces long-steroid usage.
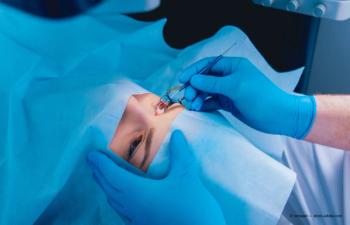
There is a lot to learn from the history of LASIK if ODs are willing to unearth it.
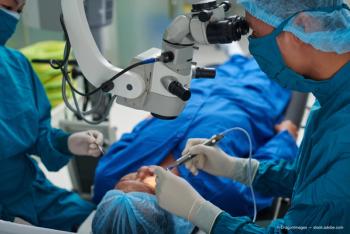



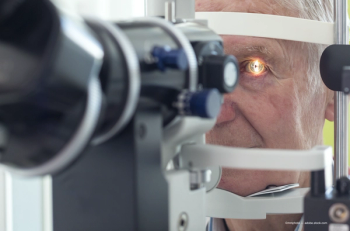

Corneal ectasia is one of the worst outcomes of laser eye surgery (LASIK). One OD takes a look at the importance of operating on good candidates and the newest technologies to do so succesfully.

Refractive surgery is no stranger to evolving technology and research. Jim Owen, OD, MBA, FAAO, explains how recent research has changed the way he positions laser vision correction with his patients.

Our patients have numerous choices regarding advanced technology and eye care. Advances range from how patients check in for an appointment to what tools a surgeon uses to dissect tissue. They all have their benefits, and all come at a cost.

How often have you heard a post-LASIK patient say his surgery “isn’t working anymore” or it has “expired?” While the corneal tissue that was ablated is gone forever, eyes can change over time, and laser vision correction does not stop time.
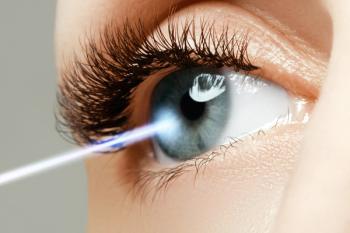
Photorefractive keratectomy (PRK) was the original excimer laser procedure approved by the FDA-and is still a safe and effective treatment of refractive errors. PRK has the benefits of no-flap creation; therefore, there is no risk of flap complications.

Prepare your patient by assessing and treating the ocular surface
As your patients celebrate another birthday milestone, they are again back in your chair wondering why their reading glasses mysteriously disappear when they are out exploring life or why their arms are not as long as they used to be.
Published: October 18th 2016 | Updated:

Published: January 30th 2017 | Updated:

Published: November 2nd 2017 | Updated:
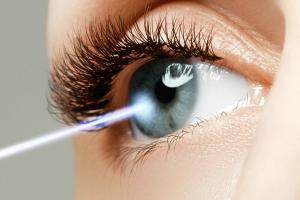
Published: April 17th 2017 | Updated:

Published: July 18th 2017 | Updated:

Published: January 29th 2018 | Updated: