OCT
Latest News
Latest Videos

Shorts

CME Content
More News
The investigators described the CASIA2 (Tomey Corporation) instrument, which is a new AS-OCT device with a swept-source laser wavelength of 1310 nm that can scan at a speed of 50,000 A-scan/second.
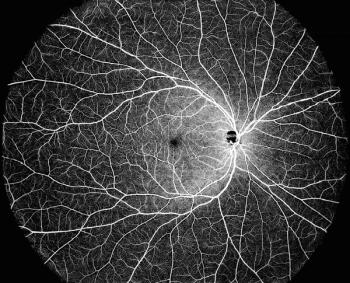
DREAM is an acronym for deep imaging depth, rapid sweeping speed, extensive scan range, accurate results, and multimodal imaging capabilities.

With the acquisition, Topcon Healthcare also assumes RetInSight’s AI algorithms that analyze retinal images to detect and monitor disease.

A total of 43 patients who recovered from the SARS-CoV-2 infection with mild pneumonia were included along with 45 healthy individuals.
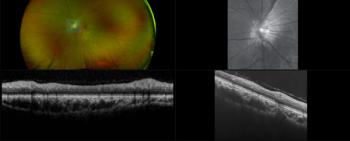
MonacoPro, the next evolution of Monaco from Optos, retains the powerful ultra-widefield SLO and spectral domain imaging while adding additional key product features.

Results from the study assisted Notal Vision in receiving De Novo authorization from the US FDA for the SCANLY Home OCT in 2024.

A recent study evaluated both deep neural networks and aggregation functions to determine ways to improve schizophrenia detection.

The primary safety endpoint was carried out through the percentage of patients with shift from normal (at baseline) to abnormal in any electrocardiogram (ECG).

Researchers described the presence of multiple bilateral serous retinal detachments (SRDs) found in 3 women after they used hair dyes.

Korean researchers developed an AI model using OCT images to predict neovascular AMD treatment outcomes after anti-VEGF injections.
The study evaluates Duravyu’s efficacy, durability, and re-dosing every 6 months in both treatment-naïve and previously treated patients.
Watching out for inevitable degenerative changes can improve patient care.

The primary findings were that a higher BMI was protective against glaucoma progression and use of tobacco and alcohol were not significantly associated with retinal nerve fiber layer change.

According to the company, the topography module now makes the OCT the only one with FDA cleared OCT-A metrics on the market.

Danica Marrelli, OD, FAAO, AAO Dip, gives advice for those looking to upgrade their OCT or integrate the device into their practice.

Mark Dunbar, OD, FAAO, details a presentation he gave alongside Rishi Singh, MD, on geographic atrophy at Vision Expo West 2024.
By identifying progressive GA earlier, primary eye care providers can make timely referrals and save patients’ visual function.

Comanagement is a key component for treatment of disease.

Case complexity underscores the importance of interdisciplinary communication.

The study helped identify predisposing factors for severe SANS in astronauts.

Utilizing artificial intelligence may provide feasibility assessments, data-driven protocol design, and cost reduction opportunities.

Notal Vision’s device was given to 15 patients to track changes in their neovascular age-related macular degeneration for the study.
Respecting the clinical importance of the pachychoroid spectrum is vital when analyzing OCT scans.

Raman Bhakrhi, OD, FAAO, said that optometrists' collaboration with primary care physicians and other medical professionals can help minimize the chance for retinal damage caused by medications.

Edmund Tsui, MD, details findings from a study that suggests that swept-source anterior segment OCT images by provide more objective ways to measure inflammation in the eye.