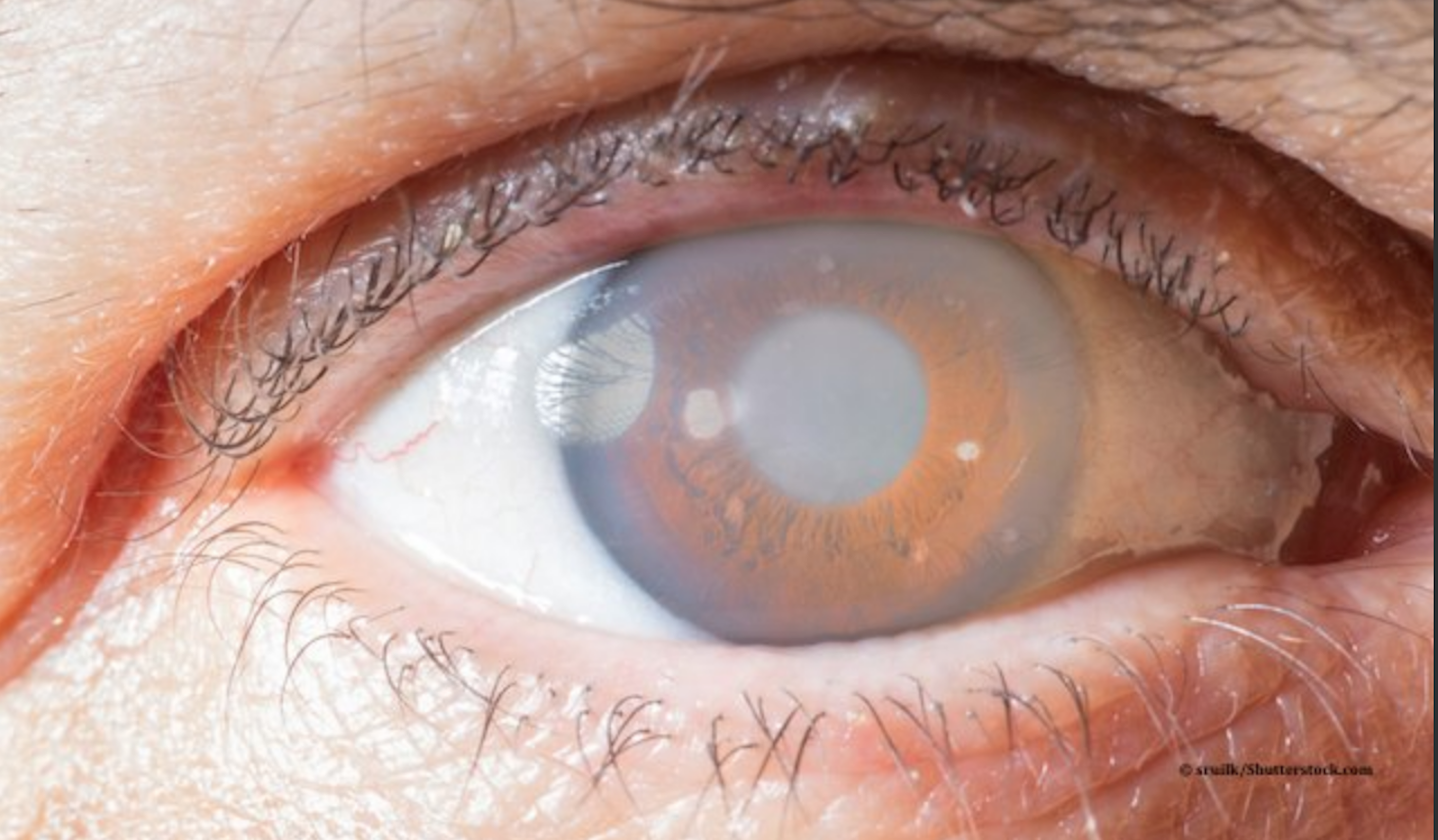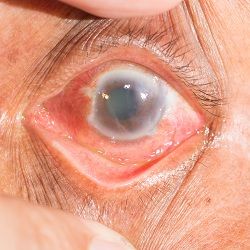
Glaucoma
Latest News
CME Content






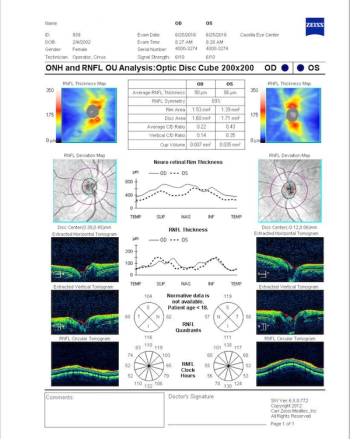

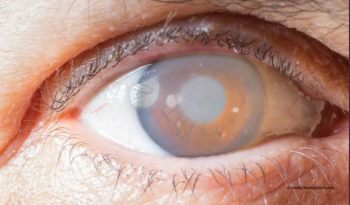

Treatments continue to evolve, and glaucoma treatments are no different. When treating glaucoma patients, it is important to stay up to date on new technologies and continue to monitor IOP.

Optometry Times Chief Optometric Editor Benjamin P. Casella, OD, FAAO, discusses how exercises including yoga impact patients who have glaucoma.

Factors such as age, family history, and race are not modifiable. One OD examines how a change in dietary habits may be beneficial in treating those suffering from glaucoma.

It is not realistic for patients to be prepared to respond when they are given news of a disease or disorder. Many times, patients are caught off guard at the mention of disease and assume a blank stare. What questions are they supposed to ask? Will Smith, OD, anticipates these questions and provides staff with information to keep patients informed.

Prescribing narcotics and opioids has come under scrutiny of late as the opioid epidemic continues to grow. Optometry Times Chief Optometric Editor Benjamin P. Casella, OD, FAAO, gives his three key points to consider before handing over that prescription to your patient.